Ad Blocker Detected
Our website is made possible by displaying online advertisements to our visitors. Please consider supporting us by disabling your ad blocker.
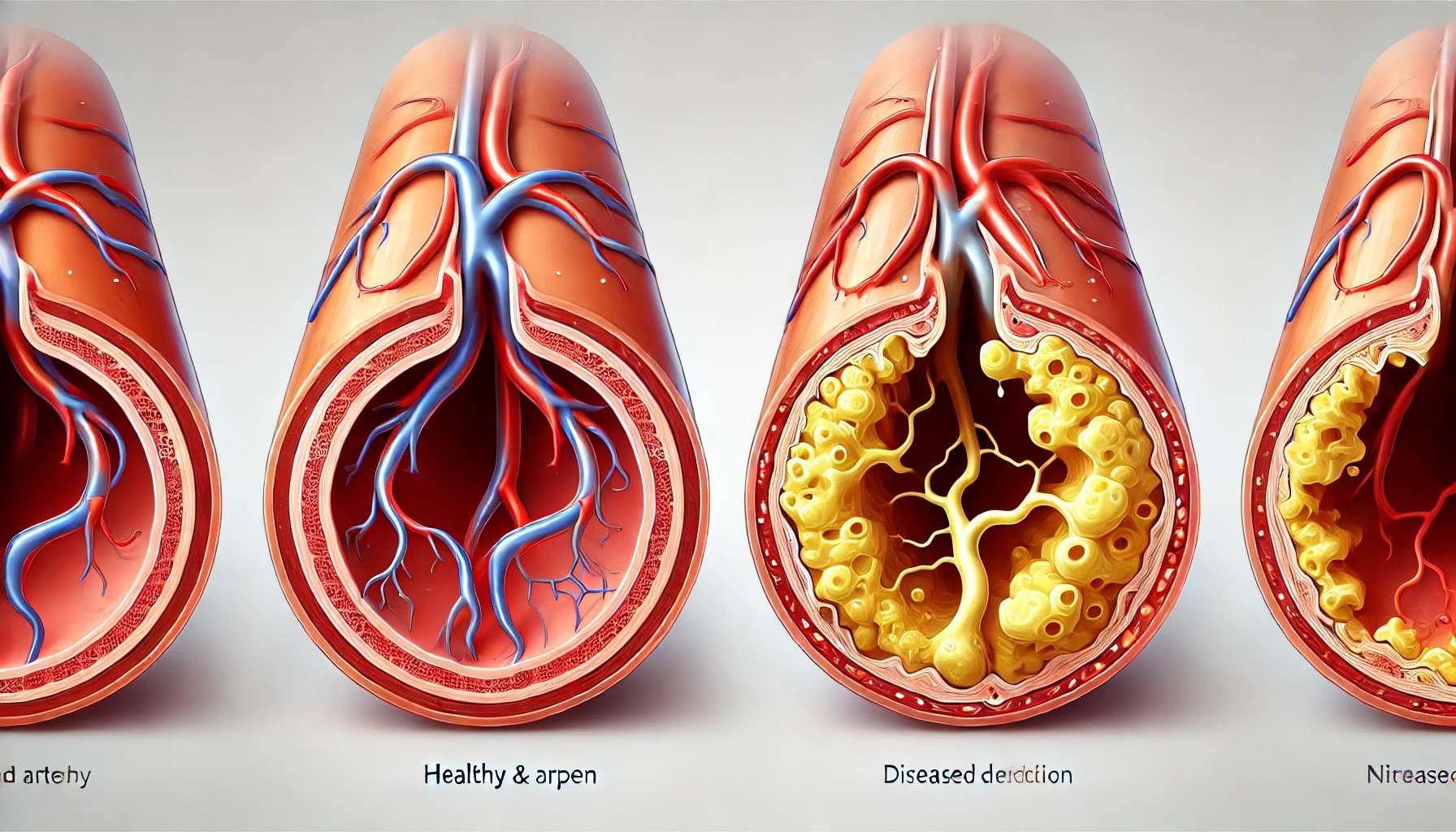
Peripheral Artery Disease (PAD)—a condition that some people poetically describe as the “traffic jam in your veins”—is not just a medical term; it’s a wake-up call for your circulatory system. Imagine a clogged highway where blood struggles to reach its destination—usually your legs. That’s PAD for you. It’s caused by fatty deposits (plaque) setting up camp in your arteries, narrowing the paths for blood to flow freely.
While PAD has no age preference, older adults seem to bear the brunt of it, especially those wrestling with health issues like diabetes or high blood pressure. Ignoring PAD? That’s like refusing to patch a leaking roof—before you know it, things could spiral into serious complications like unrelenting pain, tissue damage, or even losing a limb. Sobering, isn’t it? But hold tight; we’ll explore this condition inside out—from its subtle whispers to its loud, screaming alarms.
What’s Peripheral Artery Disease Anyway?
PAD doesn’t discriminate; it primarily impacts the arteries feeding your legs, but other areas like your arms might join the party too. At the heart of it all lies atherosclerosis—a sneaky villain where a concoction of cholesterol, fat, calcium, and other bits of cellular debris pile up in artery walls. It’s like a slow-building traffic jam, and the end result? Restricted blood flow.
When oxygen and nutrients can’t reach your limbs, you might feel anything from a faint twinge to outright agony. And let’s not sugarcoat it—if PAD goes unchecked, it might force drastic measures like amputation. Not the kind of plot twist anyone wants in their health story.
Oh, and here’s the kicker: PAD doesn’t just stroll in and stay the same. Nope, it evolves. Plaque buildup gets worse over time, like rust eating away at metal. The earlier you spot it, the better your chances of managing—maybe even slowing—this relentless progression.
Spotting the Symptoms of PAD: It’s Not Always Obvious
Some people with PAD? They breeze through life clueless, as silent as the condition can be in its early stages. But others—let’s just say they don’t get off that easy.
The most famous symptom (if PAD were a movie star) is intermittent claudication—a fancy term for leg pain or cramping that hits you like clockwork during exercise but eases up when you rest. It usually camps out in your calves but doesn’t mind wandering to your thighs, hips, or even feet.
Other signs might sound like unrelated nuisances, but they’re all pieces of the PAD puzzle:
- Ice-cold limbs: Ever feel like your feet could double as popsicles, even in July?
- Weak pulse: Sometimes, the heartbeat in your affected leg or arm feels faint—or just MIA.
- Wounds that linger: Cuts or sores take their sweet time healing because blood isn’t flowing efficiently.
- Skin drama: Pale, bluish, or downright weird skin tones might pop up.
- Hair loss: Your legs or feet could go bald—an odd thought, but it happens.
- Erectile dysfunction: For men, blood flow issues might disrupt intimacy.
But here’s the plot twist: many of these symptoms overlap with other conditions. So, self-diagnosing? That’s a recipe for confusion. A quick chat with your doctor beats a guessing game every time.
The Risky Business of Developing PAD
Let’s cut to the chase. Who’s most likely to tango with PAD? It’s not just bad luck; certain habits and conditions stack the odds against you:
- Aging gracefully—or not so much: Once you cross 60, PAD risk shoots up.
- Smoking: No surprises here—cigarettes are like steroids for plaque buildup.
- High blood pressure and cholesterol: Think of them as twin architects building your arterial roadblocks.
- Diabetes: A major player in PAD, often making things worse and more stubborn to treat.
- Couch potato syndrome: Inactivity is an underrated villain in this saga.
- Family history: Blame it on genetics if PAD runs in your bloodline.
But don’t despair; these aren’t unchangeable facts of life. Lifestyle tweaks can tip the scales in your favor—quit smoking, move more, eat better, rinse, repeat.
PAD Treatment: A Spectrum of Choices
Dealing with PAD is a mix of science and strategy. Treatments vary depending on how bad things are:
- Lifestyle overhauls: Your doctor might sound like a motivational speaker, urging you to ditch tobacco, eat clean, and get moving.
- Pills and potions: Medications tackle the usual suspects—cholesterol, blood pressure, and clotting risks.
- Sweat equity: Supervised exercise therapy isn’t just about fitness; it’s a lifeline for improving circulation.
- Angioplasty and stenting: Fancy words for minimally invasive procedures that open up stubbornly narrow arteries.
- Surgical detours: In dire cases, bypass surgery creates a workaround for blood flow.
Can We Prevent PAD Altogether?
If prevention had a motto for PAD, it’d be, “Stop the traffic jam before it starts.” Here’s how:
- Drop the smokes: Seriously, it’s non-negotiable.
- Stay active: Even small daily walks add up.
- Eat like your arteries depend on it: Think veggies, whole grains, lean proteins, and healthy fats.
- Check-in with your doctor: Regular screenings can catch PAD early, maybe even before symptoms show.
Final Thoughts
Peripheral Artery Disease isn’t just another line in your health chart. It’s a challenge, a reminder, and—if managed well—a success story waiting to be written. Whether it’s quitting cigarettes or taking that extra lap around the block, small actions can rewrite your PAD narrative.
Feeling uneasy about your risk? Reach out to your doctor—they’ll guide you better than any Google rabbit hole ever could.
Share health, spread hope.